
How Intermountain Health Drove $7M in Cost of Care Savings and Gained 2,150+ Hours With Unite Us
 Intermountain Health, the largest nonprofit health system in the Intermountain West, partnered with Unite Us in 2019 to build a coordinated, statewide network addressing patients’ non-medical needs. Through measurable gains in household income, administrative efficiency, healthcare cost savings, and expanded network reach, the partnership demonstrates how integrated care coordination infrastructure can improve outcomes for patients while reducing the total cost of care.
Intermountain Health, the largest nonprofit health system in the Intermountain West, partnered with Unite Us in 2019 to build a coordinated, statewide network addressing patients’ non-medical needs. Through measurable gains in household income, administrative efficiency, healthcare cost savings, and expanded network reach, the partnership demonstrates how integrated care coordination infrastructure can improve outcomes for patients while reducing the total cost of care.
.
Background
The Utah Alliance for the Determinants of Health is a community collaborative convened and funded by Intermountain Health with the vision of delivering a continuum of care that includes community resources, improved health outcomes, and affordable healthcare to those who need it most. In June 2019 the Alliance partnered with Unite Us, creating a centrally connected network of healthcare and community-based care providers throughout Utah.
Challenge
Prior to implementing Unite Us, Intermountain Health faced several common barriers experienced by large health systems working to effectively address drivers of health:
- Fragmented referral processes across clinical and community-based organizations
- Limited visibility into whether patients successfully received services
- Manual, time-intensive care coordination workflows
- Inconsistent data collection and reporting on care outcomes
- Difficulty quantifying the financial and clinical impact of care interventions
Without a centralized infrastructure, care teams lacked real-time feedback loops and shared accountability with community partners. This limited Intermountain Health’s ability to scale SDOH efforts, measure outcomes effectively, and demonstrate return on investment over time.
Solution
The adoption of Unite Us has provided several measurable benefits to Intermountain Health’s mission. We examined how Unite Us has made a difference to the Intermountain Health system and its patients through saved household income, administrative efficiency, estimated healthcare savings, and network reach.
Impact
Since adopting Unite Us, Intermountain Health has generated measurable impact across household stability, administrative efficiency, healthcare cost savings, and statewide network growth.
.

Household Impact
We estimate that Intermountain Health patients who were served by Unite Us generated approximately $3.6M in additional or saved household income.¹ These savings represent the value of non-medical services, like food, housing and shelter, employment, and utilities, to which Intermountain patients were connected via Unite Us.
Administrative Impact
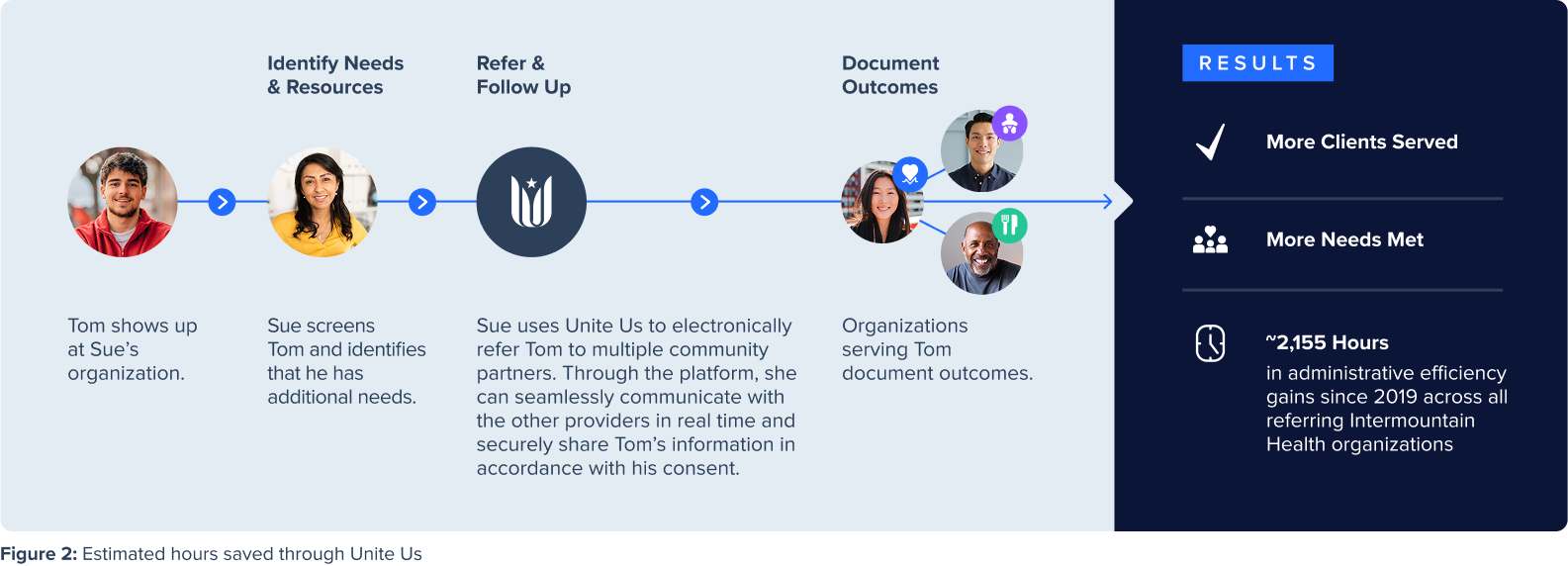
Through a prior matched longitudinal survey of 101 individuals, we found an average of 13 minutes of time savings throughout the workflow, per case, when using the Unite Us platform compared to time spent prior to implementing Unite Us. We applied that time savings to the total number cases referred by Intermountain Health organizations since the adoption of Unite Us, and estimated that 2,155 hours of administrative efficiency were gained since 2019 across all referring Intermountain Health organizations.
Healthcare Impact
We estimate that by October 2025, Intermountain Health has saved up to $7M in total cost of care for Medicaid patients.² ³ If every Intermountain Health Medicaid member was served by Unite Us, savings could have exceeded $182.4M during the same time period.
.
Service Utilization and Resolved Needs
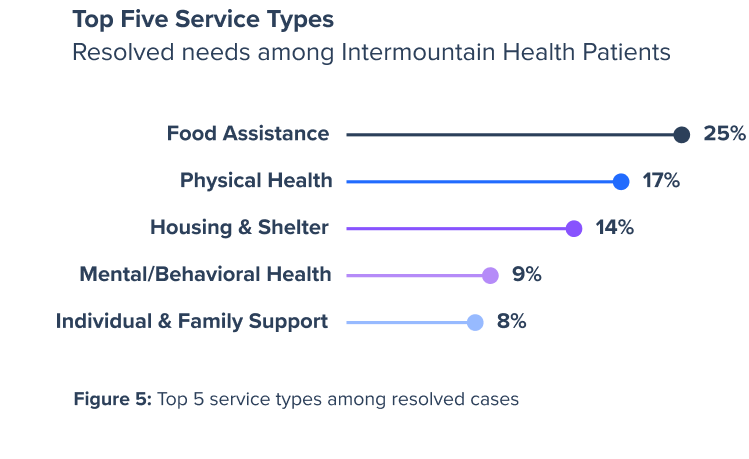 Figure 5 highlights the most common types of services accessed by Intermountain Health patients through Unite Us, illustrating where coordinated referrals most frequently resulted in resolved needs. Food assistance represented the largest share of resolved needs (25%), reflecting sustained demand for access to services such as food pantries, emergency food support, SNAP/WIC enrollment and prepared meals. Physical health-related services accounted for 17% of resolved needs. Notably; dental care accounted for 39% of all resolved physical health needs, highlighting oral health as a key area of unmet needs addressed through community-based referrals. Housing and shelter services comprised 14% of resolved needs, followed by mental and behavioral health (9%) and individual and family support services (8%).
Figure 5 highlights the most common types of services accessed by Intermountain Health patients through Unite Us, illustrating where coordinated referrals most frequently resulted in resolved needs. Food assistance represented the largest share of resolved needs (25%), reflecting sustained demand for access to services such as food pantries, emergency food support, SNAP/WIC enrollment and prepared meals. Physical health-related services accounted for 17% of resolved needs. Notably; dental care accounted for 39% of all resolved physical health needs, highlighting oral health as a key area of unmet needs addressed through community-based referrals. Housing and shelter services comprised 14% of resolved needs, followed by mental and behavioral health (9%) and individual and family support services (8%).
Network Reach
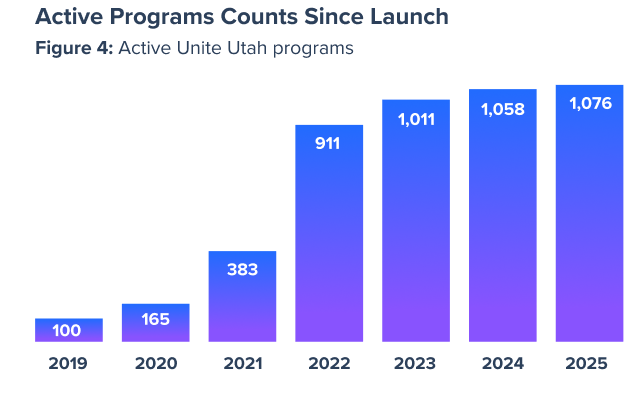
The Unite Utah network expansion has been driven largely by Intermountain Health, now connecting residents to more than 1,000 unique programs from nearly 500 on-platform, engaged partner organizations. As a direct result of this increased collaboration, patients who have been referred into the network have seen indirect benefits from Intermountain Health’s work, with an additional $1.8M in accessible income among 594 patients.⁴
Key features of the network also include the Utah Coordination Center (UCC) operated by the United Way of Salt Lake. Since 2020, the UCC has served 1,337 clients for 2,396 needs. When finding best-fit partners on the platform for client referrals, community partners have shown a 62% resolution rate in meeting their needs. In instances where a best-fit partner is not available, UCC utilizes the off-platform resources functionality of the platform. Care coordinators at the United Way of Salt Lake have a high and efficient case closure rate for these off-platform needs. 99% of all off-platform cases have been closed, and the median time to closure is within 2 weeks.
Lessons Learned
Intermountain Health’s experience illustrates how investing in technology solutions to address patients’ SDOH needs can generate meaningful financial and health outcomes at scale. By integrating healthcare and community-based services into a shared technology platform, health systems can move from screening to measurably improving patient outcomes.
Key lessons include:
- Closed-loop referrals drive accountability. Visibility into outcomes strengthens collaboration between healthcare and community partners.
- Care coordination reduces total cost of care. Addressing unmet needs contributes to significant cost savings across the health system.
- Administrative efficiency enables scale. Even modest time savings per case compound into thousands of hours saved systemwide.
- Statewide connectivity reduces fragmentation. A unified referral infrastructure results in coordinated, trackable outcomes, rather than siloed outreach efforts.
 With measurable gains in household income, administrative efficiency, and total cost of care savings, Intermountain Health’s partnership with Unite Us demonstrates that when healthcare and community partners work in coordination, meaningful impact follows—for patients, providers, and entire communities.
With measurable gains in household income, administrative efficiency, and total cost of care savings, Intermountain Health’s partnership with Unite Us demonstrates that when healthcare and community partners work in coordination, meaningful impact follows—for patients, providers, and entire communities.
About Unite Us
Unite Us is the nation’s leading software company bringing sectors together to improve the health and well-being of communities. We drive the collaboration to identify, deliver, and pay for services that impact whole-person health. Through Unite Us’ national network and software, community-based organizations, government agencies, and healthcare organizations are all connected to better collaborate to meet the needs of the individuals in their communities.






